Common Skin Conditions
Clinical Dermatology consists of the evaluation and treatment of skin conditions and skin disease. West Michigan Dermatology’s high level clinical dermatology competence is of great comfort to patients of all ages seeking diagnosis and treatment of common or rare skin conditions.
Skin is a complex organ and is susceptible to many issues. Some concerns, of course, are more common than others. Skin may develop rashes, color and/or textural changes as well as both harmless and cancerous growths. The key to management of skin conditions, whether common or rare, is proper diagnosis followed by carefully considered patient-specific treatment.
As with all medical issues, optimal skin treatment results from synergy of science and art. One size does not fit all with clinical dermatology. Differences in dermatology expertise and practice patterns result in significant real world variations in patient outcomes. Our ongoing commitment is to provide the best attainable clinical outcomes for our patients.
Acne
Acne is a common skin condition that affects mostly teenagers, but is not limited to just that age category. 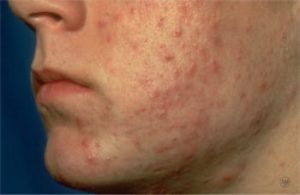 It also can affect adults even into their 40’s. Acne can clear up after a few years even if it goes untreated, but this can lead to severe lifelong scars that can affect a person’s self image. There is no reason to not treat acne since there are many different methods that will control and even cure the acne.
It also can affect adults even into their 40’s. Acne can clear up after a few years even if it goes untreated, but this can lead to severe lifelong scars that can affect a person’s self image. There is no reason to not treat acne since there are many different methods that will control and even cure the acne.
Acne consists of blackheads, whiteheads, pimples, and sometimes deeper boil-like lesions called nodules. Acne usually occurs on the face, but it can also show up on the back, chest, shoulders and neck. While acne is not a life threatening condition, it can be very upsetting and disfiguring. When it is in its severest stage, it can lead to serious and permanent scarring. Even less severe cases have been known to scar also.
How Acne forms:
Rising hormone levels during puberty cause the sebaceous (oil) glands of the skin to get larger. This growth occurs in areas where acne is most common (the face, upper back and chest. It is activated by male-type hormones found in both males and females.
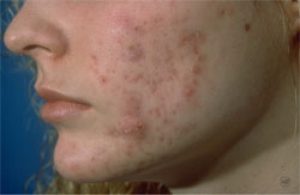 These sebaceous glands make an oily substance called sebum which reaches the surface by emptying through the opening of the follicle on to the skin surface. The glands are connected to a hair-containing canal called a follicle. The oil’s material seems to stimulate the lining of the wall of the follicle. The cells shed more rapidly and stick together, plugging the openings of the skin surface. Also, the mixture of oil and cells help bacteria in the follicles grow.
These sebaceous glands make an oily substance called sebum which reaches the surface by emptying through the opening of the follicle on to the skin surface. The glands are connected to a hair-containing canal called a follicle. The oil’s material seems to stimulate the lining of the wall of the follicle. The cells shed more rapidly and stick together, plugging the openings of the skin surface. Also, the mixture of oil and cells help bacteria in the follicles grow.
These bacteria produce chemicals that cause the wall of the follicle to break. When the wall is broken, sebum, bacteria and shed skin cells escape. This is the process by which pimples and large bumps are formed.
Cleansing:
Acne is not a disease caused by dirt. Blackheads are not dirt, but are due to dried oil and shed skin cells in the openings of the hair follicles. You should wash your face with soap and warm water twice a day. It’s important not to wash too often as this may aggravate acne. Shampooing on a regular basis is also recommended. You should wash hair more often if it tends to be oily. A dermatologist can assist you with the best face and hair washing products and routine.
Diet:
There are differing opinions regarding diet and the relationship to acne. It is not the primary cause of acne. It cannot be cured by following any type of strict diet, although some people feel their acne tends to get worse with certain foods.
Sunlight:
Some people see an improvement in their acne by being out in the sun. However, this is only temporary. 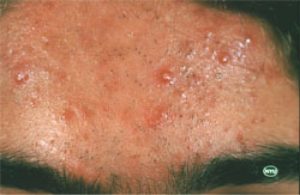 Actually, prolong sun exposure can make the acne worse and too much sun exposure can cause premature aging and skin cancer.
Actually, prolong sun exposure can make the acne worse and too much sun exposure can cause premature aging and skin cancer.
Treatment:
Treatment of acne should begin with an evaluation with a Dermatologist. They will first find out if your skin condition is routine acne. Sometimes, people have an acne like rash due to outside elements, such as makeup or lotion or even oral medications.
Some non-prescription acne lotions and creams can help very mild cases of acne, but used to often will tend to dry out the skin. If you are looking for over-the-counter acne products, make sure it is “non-comedogenic”. This means that using this product should not cause whiteheads or blackheads. Makeup should be removed every night with soap and water.
There are prescription creams and lotions plus antibiotics taken by mouth that are very successful in treating moderate to severe acne. The antibiotics are used to reduce the bacteria in the follicle. In severe cases, there are different oral medications that are used that will help the acne if other medications have failed. Accutane is one of these medications but the patient has to adhere to strict regulations and must understand the side effects of the drug. Frequent follow ups are mandatory and prevention of pregnancy in females is a must, since the drug can cause severe birth defects.No matter what treatment you decide to use, you must continue proper skin care. There is no instant or permanent cure for acne, but it is controllable.
Moles
Everyone has moles, sometimes 40 or more. Most people think of a mole as a dark brown spot, but moles have a wide range of appearances.
Moles can appear anywhere on the skin. They are usually brown in color but can be skin colored and various shapes and sizes. The brown color is caused by melanocytes, special cells that produce the pigment melanin. Most moles appear during the first 20 years of life, although some may appear later on. Sun exposure increases the number of moles, and they may darken.
Each mole has its own growth pattern. The typical life cycle of a common mole takes about 50 years. Recent studies have shown that certain types of moles have a high-than-average risk or becoming cancerous. They may develop into a form of skin cancer known as malignant melanoma. Sunburns may increase the risk of melanoma.
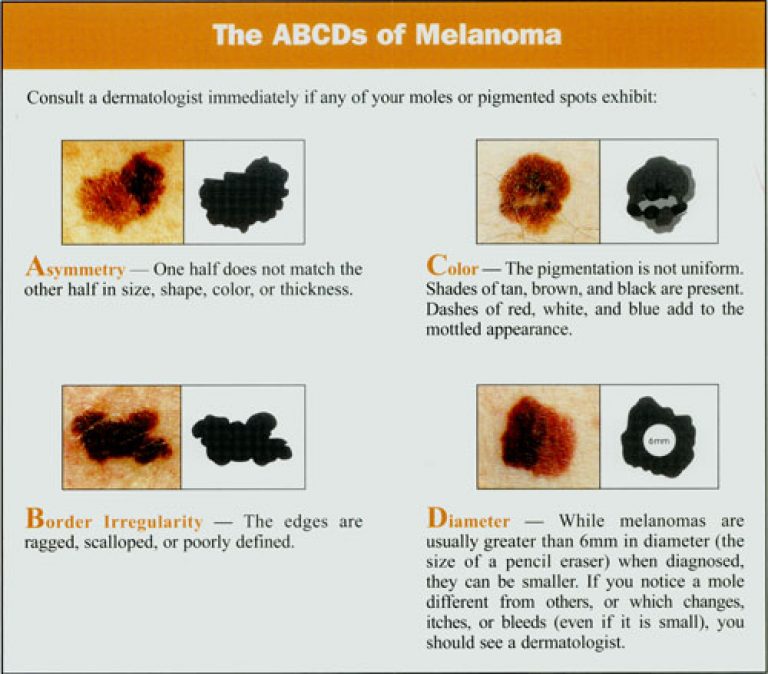
Moles are present at birth and these are called congenital nevi. These moles have a greater tendency to develop into melanoma. Moles known as dysplastic nevi or atypical moles are larger than average (usually larger than a pencil eraser) and irregular in shape. They tend to have uneven color with dark brown centers and a lighter, sometimes reddish, uneven border or black dots at edge. People with dysplastic nevi may have a greater change of developing malignant melanoma and should be seen regularly by a dermatologist to check for any changes. They also need to learn to do self-examinations, looking for changes in the color, size or shape of their moles, or the appearance of new moles.
The majority of moles and other blemishes are benign (non-cancerous). They will never be a threat to the health of the person. Spots or blemishes that warrant medical concern are those that do something out of the ordinary-those that act differently from other existing moles. This includes any spot that changes in size, shape, color, bleeds, itches, becomes painful, or moles that appear when a person is past twenty.
If you notice a mole that does not follow the normal patterns, a dermatologist may be able to assure you that the mole is harmless, or confirm that it is cancerous. He or she may remove the mole or part of it (biopsy) to study it under a microscope. If the growth was only partially removed and it is found to be cancerous, then the entire lesion and an extra margin of safety will need to be removed.
A person may wish to get rid of moles that are irritating them, or simply because they are unattractive. The most common methods of removal include numbing and shaving the mole off, or cutting out the entire lesion and stitching the area closed.
Most moles cause no problems. But occasionally a mole may be unattractive, annoying or changing. If you see any signs of change or want a mole removed for cosmetic reasons, consult a dermatologist.
Skin Cancer
Skin cancer is the most prevalent of all types of cancers. It is estimated that more than one million Americans develop skin cancer every year.
Fair skinned people who sunburn easily are at a particularly high risk for developing skin cancer. Other less important factors include repeated medical and industrial x-ray exposure, scarring from diseases or burns, occupational exposure to compounds such as coal tar and arsenic, and family history.
The best defense against skin cancer is sun avoidance. Overexposure to ultraviolet light (sunlight or tanning beds), especially if it results in sunburn and blistering, is the main cause of skin cancer. Protecting the skin from the sun’s ultraviolet rays is the best way to protect yourself from skin cancer.
Common Types of Skin Cancer:
Actinic Keratoses
Actinic Keratoses or solar keratoses are considered the earliest stage in the development of skin cancer. 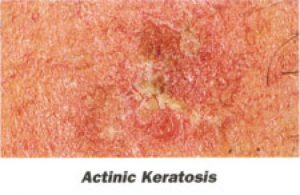 They are small, scaly spots most commonly found on the face, ears, neck, lower arms, and back of the hands in fair-skinned individuals who have had significant sun exposure Some actinic keratoses may progress to advanced stages which require more extensive treatment. Proper use of sunscreens can help prevent actinic keratoses even after extensive sun damage has already occurred.These lesions can be treated by cryotherapy (freezing), topical chemotherapy (applying a cream or lotion), chemical peeling, dermabrasion, laser surgery, and curettage.
They are small, scaly spots most commonly found on the face, ears, neck, lower arms, and back of the hands in fair-skinned individuals who have had significant sun exposure Some actinic keratoses may progress to advanced stages which require more extensive treatment. Proper use of sunscreens can help prevent actinic keratoses even after extensive sun damage has already occurred.These lesions can be treated by cryotherapy (freezing), topical chemotherapy (applying a cream or lotion), chemical peeling, dermabrasion, laser surgery, and curettage.
Basal Cell Carcinoma
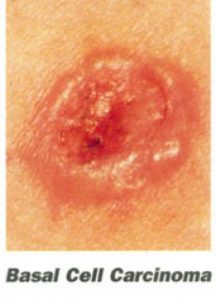
Basal cell carcinoma is the most common type of skin cancer and appears frequently on the head, neck and 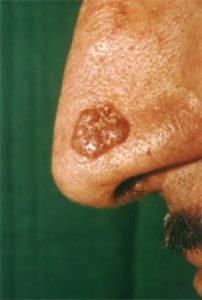 hands as a small, fleshy bump, nodule or red patch. Other parts of the body may be affected as well. Fair-skinned people are more prone to basal cell carcinomas. This type of cancer is rarely found in dark-skinned people. They do not spread quickly. It can take many months or years for one to grow to a diameter of one-half inch. Untreated, the cancer often will begin to bleed, crust over, heal and then repeat this process.
hands as a small, fleshy bump, nodule or red patch. Other parts of the body may be affected as well. Fair-skinned people are more prone to basal cell carcinomas. This type of cancer is rarely found in dark-skinned people. They do not spread quickly. It can take many months or years for one to grow to a diameter of one-half inch. Untreated, the cancer often will begin to bleed, crust over, heal and then repeat this process.
 This type of skin cancer very seldom metastasizes (spreads to other parts of the body), but it can extend below the skin to the bone and nerves, causing considerable local damage.
This type of skin cancer very seldom metastasizes (spreads to other parts of the body), but it can extend below the skin to the bone and nerves, causing considerable local damage.
Treatment options include excision, topical chemotherapy, immune therapy, curettage and electrodessication and MOHS micrographic surgery.
Squamous Cell Carcinoma
Squamous cell carcinoma is the second most common skin cancer. It again is found mostly in fair-skinned 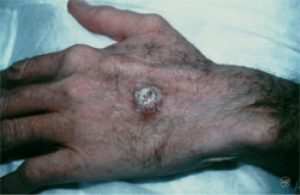 people, but very seldom in dark-skinned people. These are more commonly found on the rim of the ear, the face, lips, and mouth. This type of cancer may appears as a bump, or as a red, scaly patch. Squamous cell CA may turn into large masses and become invasive. Unlike basal cell carcinoma, this form of cancer can metastasize (spread to other parts of the body). Early diagnosis and treatment is essential. When found early and treated properly, the cure rate for both BCC and SCC is more than 95 percent.Treatment options include excision, topical chemotherapy, immune therapy, curettage and electrodessication, and MOHS micrographic surgery.
people, but very seldom in dark-skinned people. These are more commonly found on the rim of the ear, the face, lips, and mouth. This type of cancer may appears as a bump, or as a red, scaly patch. Squamous cell CA may turn into large masses and become invasive. Unlike basal cell carcinoma, this form of cancer can metastasize (spread to other parts of the body). Early diagnosis and treatment is essential. When found early and treated properly, the cure rate for both BCC and SCC is more than 95 percent.Treatment options include excision, topical chemotherapy, immune therapy, curettage and electrodessication, and MOHS micrographic surgery.
Malignant Melanoma
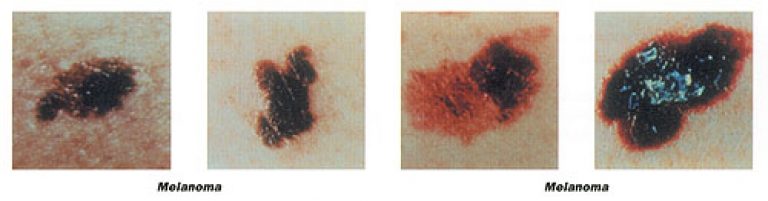
Malignant Melanoma is the most deadly of all skin cancers. It is estimated that 7,700 Americans will die from melanoma and that 46,000 Americans will develop this type of skin cancer. The death rate is declining because melanoma is usually curable when detected in its early stages and patients are seeking help sooner.Excessive sun exposure, especially sunburn is the most probable cause for melanoma. Light-skinned individuals are at particular risk, although dark skin is not a guarantee against melanoma. Heredity also plays a part since you have an increased chance of developing melanoma if a relative or close family member has had melanoma.
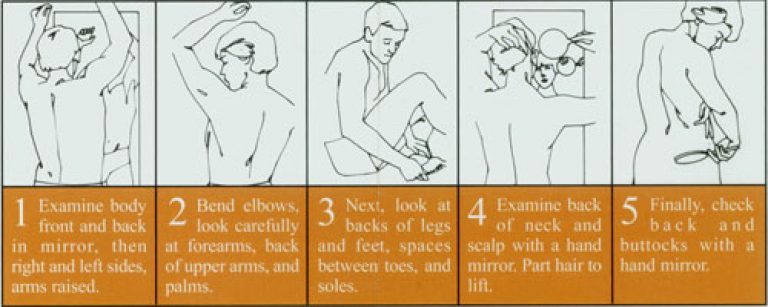
Periodic Self-Examination:
Early detection and removal offer the best chance for a cure. Periodic self-examinations aid in recognition of any new or developing lesion. Get familiar with your skin and your own pattern of moles, freckles, and “beauty marks.” Make sure to look at the entire body every month or two. Watch for changes in the number, size, shape, and color of pigmented areas. Consult a dermatologist promptly if any changes are noticed. Individuals at high risk should be examined by a dermatologist on a regular basis.
Hair Loss
Hair has been called our “crowning glory”. Society has placed a great deal of social andcultural importance 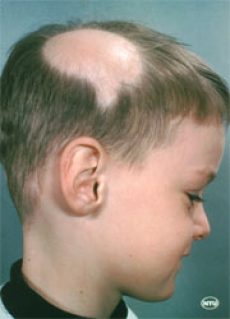 on hair and hairstyles. Unfortunately, many conditions, diseases, and improper hair care result in excessive hair loss. People who notice their hair shedding in large amounts after combing or brushing, or whose hair becomes thinner or falls out, should consult a dermatologist. With correct diagnosis, many people with hair loss can be helped.
on hair and hairstyles. Unfortunately, many conditions, diseases, and improper hair care result in excessive hair loss. People who notice their hair shedding in large amounts after combing or brushing, or whose hair becomes thinner or falls out, should consult a dermatologist. With correct diagnosis, many people with hair loss can be helped.
Dermatologists who specialize in the medical, surgical, and cosmetic treatment of diseases of the hair and skin, can evaluate a patient’s hair problem by asking questions about medical disorders and recent illnesses, diet and exercise, medications and vitamins including health food taken in the last six months, family history of hair loss, and hair care habits. Hormonal effects may be evaluated in women by asking about menstrual cycles, pregnancies and menopause. After examining the scalp and hair, the dermatologist may check a few hairs under the microscope. Sometimes blood tests or a scalp biopsy may be required for an accurate diagnosis. It’s important to find the cause of the problem and how it will respond to medical treatment.
Causes of Excessive Hair Loss :
Improper Hair Cosmetic Use/Improper Hair Care
Hereditary Thinning or Balding
Alopecia Areata
Childbirth
High Fever, Severe infection, Severe Flu
Thyroid Disease
Fungus Infection of theScalp (Ringworm)
Inadequate protein in Diet
Birth Control Pills
Low Serum Iron
Major Surgery/Chronic
Illness/Stressful Event
Hair Pulling
Cancer Treatments
Medications
As you can see, excessive hair loss can have many different causes. Hair will regrow spontaneously in some forms of hair loss. Other forms can be treated successfully by a dermatologist. Research is ongoing and is quite promising in the field of hair loss.
Warts
What are Warts?
Infantile Eczema:Warts are non-cancerous skin growths caused by a viral infection in the top layer of the 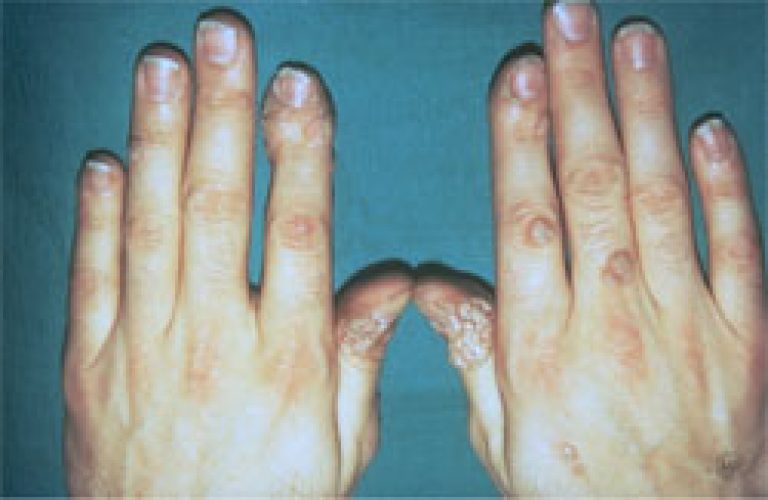 skin. Viruses that cause warts are called human papilloma virus (HPV). Warts are usually skin-colored and feel rough to the touch, but they can be dark, flat and smooth. The appearance of a wart depends on where it is growing.
skin. Viruses that cause warts are called human papilloma virus (HPV). Warts are usually skin-colored and feel rough to the touch, but they can be dark, flat and smooth. The appearance of a wart depends on where it is growing.
There are three types of warts:
*Common warts
*Foot (plantar) warts
*Flat warts
How Do You Get Warts?
 Warts are passed from person to person sometimes indirectly. The time from the first contact to the time the warts have grown large enough to be seen is often several months. The risk of catching hand, foot or flat warts from another person is very minimal.
Warts are passed from person to person sometimes indirectly. The time from the first contact to the time the warts have grown large enough to be seen is often several months. The risk of catching hand, foot or flat warts from another person is very minimal.
How Do Dermatologists Treat Warts?
Dermatologists are trained to use a variety of treatments, depending on the age of the patient and the type of wart they have. Some of the most common types of treatment are:
Salicyolic acid gel, solution or plaster.
Cantharidin
Cryotherapy (freezing)
Electrosurgery (burning)
Laser Treatment
Injection with Bleomycin
Immnotherapy
Interferon injection
Can I Treat My own Warts?
There are some wart remedies available without a prescription. However, you might mistake another kind of skin growth for a wart, and end of up treating something more serious as though it were a wart. If you have any questions about either the diagnosis or treatment, you should consult your Dermatologist.
Psoriasis
Psoriasis is a persistent skin disease that got its name from the Greek word for “itch”. The skin becomes 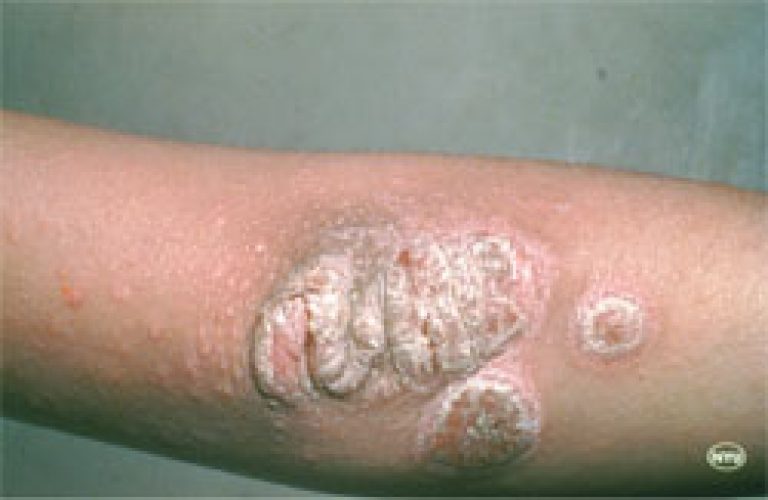 inflamed, producing red, thickened areas with silvery scales, most often on the scalp, elbows, knees and lower back.
inflamed, producing red, thickened areas with silvery scales, most often on the scalp, elbows, knees and lower back.
Psoriasis cannot be passed from one person to another, though it is considered to be a familial hereditary type disease.
Types of psoriasis:
Psoriasis comes in many forms. Each differs in how bad it is, how long it lasts, where it is, and in the shape and pattern of the scales. The most common form begins with little red bumps. Gradually these bumps grow larger and scales form. The top scales flake off easily and often but the scales below the surface stick together. When they are removed, the tender, exposed skin bleeds. These small red areas then grow, sometimes becoming quite large.
About 7% of psoriasis patients also have arthritis, which fortunately, is not too severe in most people. In some people however, the arthritis is worst when the skin is very involved. Sometimes the arthritis improves when the condition of the patient’s skin improves.
How Is Psoriasis Diagnosed?
Dermatologists diagnose psoriasis by examining the skin, nails, and scalp. They may need to do a skin biopsy to examine the tissue under the microscope.
How is Psoriasis Treated?
Treatment of psoriasis is based on the patient’s health, age, lifestyle, and the severity of the psoriasis. The goal is to reduce inflammation and to slow down rapid skin cell division. Moisturizing creams and lotions loosen scales and help control itching. Special diets have not been successful in treating psoriasis. Your dermatologist may prescribe medications to apply on the skin containing cortisone, cortisone-like compounds, synthetic Vitamin D, tar, or anthralin. These may be used in combination with natural sunlight or ultraviolet light. The most severe forms or psoriasis may require oral medications, with or without light treatment.
Sunlight exposure helps the majority of people with psoriasis but is must be used cautiously. Ultraviolet light therapy may be given in a dermatologist’s office, a psoriasis treatment center or a hospital.
New therapies under investigation include “biologic agents” that attack the abnormal immune cells that lend to psoriasis.
Your Dermatologist will decide which treatment fits you best.
Eczema/Atopic Dermatitis
The term “eczema” or dermatitis” are used to describe certain kinds of inflamed skin conditions including 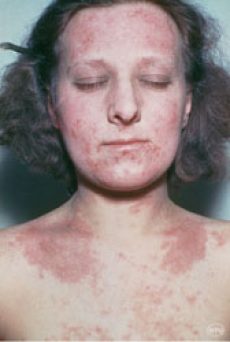 allergic contact dermatitis and nummular dermatitis. Eczema can be red, blistering, oozing, scaly, brownish, or thickened and usually itches. A special type is called atopic dermatitic or atopic eczema.
allergic contact dermatitis and nummular dermatitis. Eczema can be red, blistering, oozing, scaly, brownish, or thickened and usually itches. A special type is called atopic dermatitic or atopic eczema.
The word “atopic” means there is a tendency for excess inflammation in the skin and linings of the nose and lungs. This often runs in families with allergies such as hay fever and asthma, sensitive skin, or a history of atopic dermatitis.
Atopic eczema/dermatitis can occur at any age but is most common in infants to young adults. The skin rash is very itchy and can be widespread, or limited to just a few areas. The condition usually improves with adolescence, but many patients are affected throughout life, although not as severely as in early childhood.
Infantile Eczema:
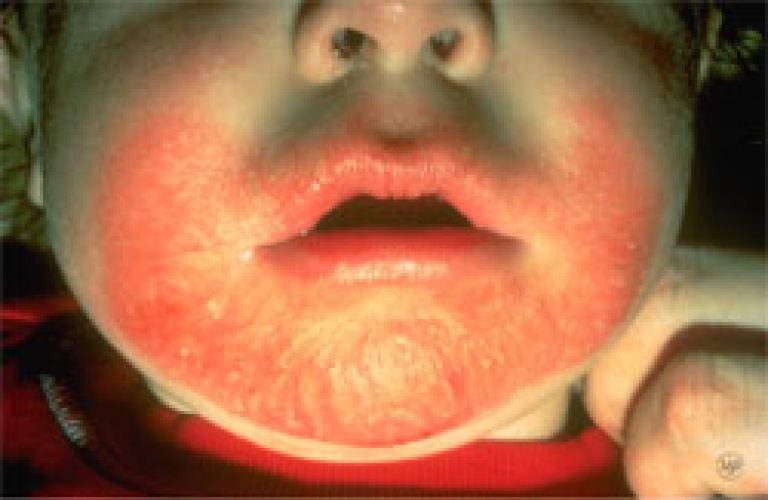 When this condition starts in infancy, it is characterized by an itchy, oozing, crusting rash and occurs mainly on the face and scalp, but patches can appear anywhere. Many babies improve before two years of age. Proper treatment can help until time solves the problems.
When this condition starts in infancy, it is characterized by an itchy, oozing, crusting rash and occurs mainly on the face and scalp, but patches can appear anywhere. Many babies improve before two years of age. Proper treatment can help until time solves the problems.
Eczema in Later life:
In teens and young adults, the patches typically occur on the hands and feet. However, any area such as the bends of the elbows, back of the knees, ankles, wrists, face, neck, and upper chest may be affected.
Other eczema patches in this stage are typically dry, red to brownish-gray, and may be scaly or thickened. The thickened areas may last for years without treatment. The intense, almost unbearable itching can continue and may be most noticeable at night. Some patients scratch the skin until it bleeds and crusts. When this occurs, the skin can get infected.
Since the disease does not always follow the same pattern, proper, early and regular treatment can bring relief and may reduce the severity and duration of the disease.
You should consult your dermatologist for advice on avoiding irritating factors in creams and lotions; 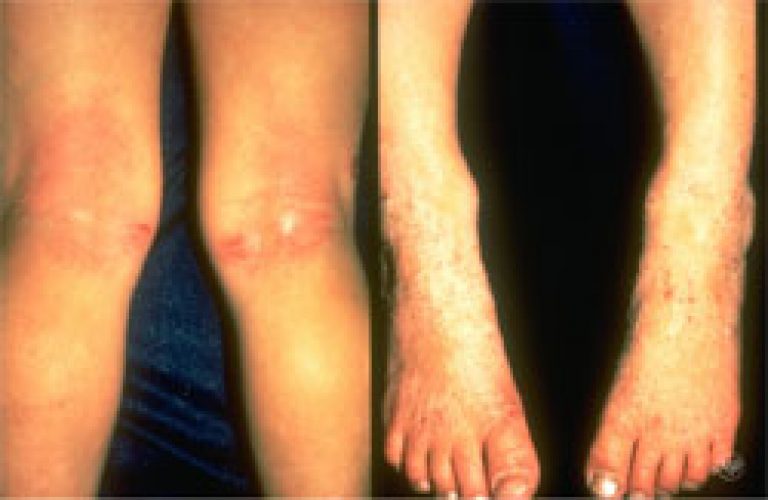 rough, scratchy or tight clothing; and woolens. Rapid changes of temperature and any activity that causes sweating can aggravate this condition. Proper bathing, moisturizing, and dealing with emotional upsets which may make the condition worse can be discussed.
rough, scratchy or tight clothing; and woolens. Rapid changes of temperature and any activity that causes sweating can aggravate this condition. Proper bathing, moisturizing, and dealing with emotional upsets which may make the condition worse can be discussed.
Your dermatologist can prescribe external medications such as steroids and newer immune modifying creams. Internal medications such as antihistamines can help with the itch. Oral antibiotics may be prescribed if there is a secondary infection. For severe cases, your dermatologist may recommend ultraviolet light treatments.
Atopic eczema/dermatitis is a very common condition. With proper treatment, the disease can be controlled in the majority of people.
Rosacea
Rosacea is a common skin disease that causes redness and swelling on the face. Often referred to as “adult acne”, rosacea may begin as a tendency to flush or blush easily, and progress to persistent redness in the center of the face that may gradually involve the cheeks, forehead, chin and nose. It may also involve the ears, chest and back. As the disease progresses, small blood vessels and tiny pimples begin to appear on and around the reddened area; however, unlike acne, there are no blackheads.
How to Recognize Rosacea: 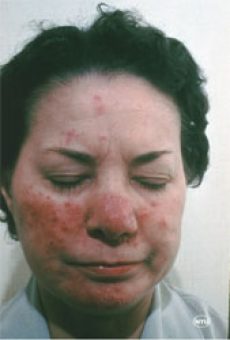
Pimples of rosacea appear on the face as small, red bumps, some of which may contain pus. These may be accompanied by the development of many tiny blood vessels on the surface of the skin and persistsent redness of the face.
Do’s & Don’ts for Rosacea Patients:
*Avoid hot drinks, spicy foods, caffeine and alcoholic beverages.
*Practice good sun protection using at least a sunscreen with SPF15
*Avoid rubbing, scrubbing or massaging the face.
*Exercise in a cool environment. Don’t overheat.
*Avoid irritating cosmetics and facial products.
*Keep a diary of flushing episodes and note associated foods, products,
activities, medications or other triggering factors.
Treatment Options:
Dermatologists often recommend a combination of treatments tailored to the individual patient. Together these treatments can stop the progress of rosacea and sometimes reverse it.
The key to successful management of rosacea is early diagnosis and treatment. It is also important to follow all of your dermatologist’s instructions. Rosacea can be treated and controlled if medical advice is sought in the early stages. When left untreated, rosacea will get worse and may be more difficult to treat.
